Night Sweats: Perimenopause or Insulin Resistance?
The mystery of night sweats
Waking up drenched in sweat, in some kind of malaise, a bit annoyed, only to feel chilled moments later, can be both frustrating and confusing. If you’re in your 40s or early 50s, you might assume night sweats are just another sign of perimenopause. But what if there’s more to the story?
Night sweats are a common symptom of perimenopause, but they can also be a red flag for insulin resistance—a metabolic imbalance that often is undetected until well confirmed. According to the Australian Bureau of Statisitics 17 to 35% of Australian adults have some degree of insulin resistance (1). Potentially 1 adult in 3!! In my opinion, more than that. The two conditions can coexist, making it tricky to pinpoint the root cause. The good news? Both can be addressed naturally through diet, lifestyle adjustments, and targeted supplements.
In this article, we’ll explore:
How perimenopause and insulin resistance each contribute to night sweats
Key differences in their underlying mechanisms
Natural strategies to support your body, whether the cause is hormonal, metabolic, or both
Perimenopause and night sweats: The hormonal connection
Perimenopause, the transitional phase before menopause, is marked by fluctuating levels of oestrogen and progesterone. These hormonal shifts disrupt your body’s internal thermostat, leading to hot flashes and night sweats.
Why it happens
Oestrogen’s role: Oestrogens help regulate serotonin and norepinephrine, neurotransmitters that influence your body’s temperature control. When oestrogens levels drop or spike erratically, your brain’s hypothalamus misinterprets signals, triggering a heat response.
Progesterone’s calming effect: Progesterone has a natural calming effect. As its levels decline relative to estrogen, the body becomes more prone to overheating (2).
Stress and Cortisol: Perimenopausal symptoms often coincide with increased stress, whether it is intense times at work or at home between elderly parents and teenagers, the stresses of life should not be underestimated. High cortisol resulting from stress, especially without supportive coping strategies, can further destabilise blood sugar (3) and/or the progesterone: oestrogen ratio (4) and exacerbate night sweats.
Typical Patterns
Night sweats often occur in the early morning hours (2–4 AM).
They may be accompanied by other perimenopausal symptoms like mood swings, irregular periods, or sleep disturbances.
Insulin Resistance and Night Sweats: The metabolic link
Insulin resistance occurs when your cells become less responsive to insulin, forcing your pancreas to produce more. Over time, this leads to high blood sugar, inflammation, and hormonal imbalances—all of which can trigger night sweats.
Why It Happens
Blood sugar crashes: If your blood sugar drops too low at night (reactive hypoglycemia), your body releases adrenaline and cortisol to stabilise it. These stress hormones can trigger a fight-or-flight response, including sweating.
Inflammation: Insulin resistance is closely tied to chronic low-grade inflammation, which can overstimulate your sympathetic nervous system, leading to overheating.
Weight and fat distribution: Excess abdominal fat, common in insulin resistance, acts like an endocrine organ, producing hormones that disrupt temperature regulation.
Typical Patterns
Night sweats may occur after a high-carb or sugary meal in the evening.
They may be accompanied by fatigue after meals, sugar cravings, or difficulty losing weight—classic signs of insulin resistance.
Unlike perimenopausal night sweats, these may improve with blood sugar stabilisation.
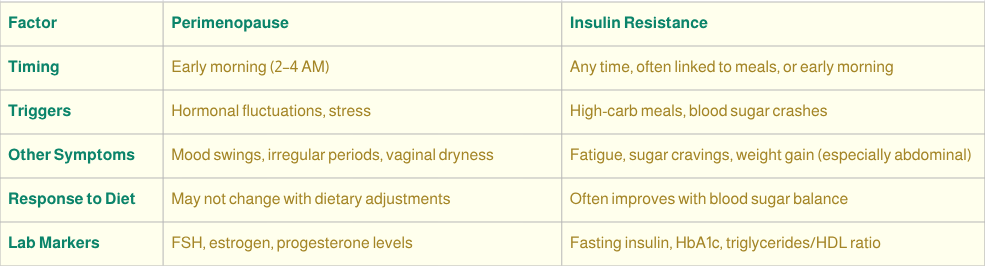
Perimenopause vs. Insulin Resistance: How to tell the difference
While both conditions can cause night sweats, there are clues to help you identify the primary culprit:
Clues related to your night sweats may overlap and be unclear. Consult your naturopath to help you navigate the uncertainties and support your body in these transitions. Further testing may be required to tailor your treatment plan.
Overlap Alert: Many women in perimenopause also develop insulin resistance due to oestrogen’s role in insulin sensitivity. Oestrogen helps cells respond to insulin, so its decline can worsen metabolic function.
Natural Solutions: Diet, Lifestyle, and Supplements
The good news? Whether your night sweats stem from perimenopause, insulin resistance, or both, natural approaches can restore balance. Here’s how to tackle each root cause—and support your body holistically.
1. Diet: Stabilise Blood Sugar and Hormones
For Insulin Resistance
Prioritise Protein and Healthy Fats: Include sources such as wild-caught fish, grass-fed meat, eggs, avocados, nuts, and seeds with every meal to slow glucose absorption.
Fibre-Rich Foods: Aim for 30g of fibre daily from vegetables, legumes, fruits, chia seeds, and flaxseeds to improve insulin sensitivity.
Low-Glycemic Carbs: Choose non-starchy vegetables, sweet potatoes, quinoa, and legumes over refined carbs.
Cinnamon and Berberine: These spices and herbs mimic insulin and help lower blood sugar. Add cinnamon to your morning tea or consider a berberine supplement.
Avoid Evening Carbs: Reduce or eliminate grains, sugars, and starchy foods after 4 PM to prevent nighttime blood sugar crashes.
For Perimenopause
Phytoestrogenic Foods: Flaxseeds, sesame seeds, tempeh, and fermented soy (like miso) can gently support estrogen balance.
Cruciferous Vegetables: Broccoli, kale, and Brussels sprouts help metabolise excess estrogen via the liver.
Omega-3s: Wild salmon, sardines, and walnuts reduce inflammation and support brain health, which can ease hormonal fluctuations.
Magnesium-Rich Foods: Spinach, pumpkin seeds, and dark chocolate (85%+) help regulate cortisol and improve sleep quality.
For Both
Hydration: Drink 2L of water daily in small amounts throughout the day to support cellular hydration.
Limit alcohol and caffeine: Both can disrupt blood sugar and worsen hot flashes. Opt for herbal teas like peppermint or chamomile.
2. Lifestyle: Cool the body and calm the nervous system
For Insulin Resistance
Aim for a 12-hour fast between dinner and breakfast: this will help give your body a rest, particularly your pancreas.
Strength training: Muscle is metabolically active and helps regulate blood sugar. Aim for 2–3 sessions per week (bodyweight exercises, resistance bands, or weights, something fun that helps you stick with it).
Post-meals walks: A 10–15 minute walk after meals can lower blood sugar spikes by up to 30%.
For Perimenopause
Sleep routine: Keep your bedroom cool (18–20°C) and dark. Use breathable fabrics (like bamboo or linen) for pyjamas and bedding.
Layered clothing: Wear light, moisture-wicking layers to bed so you can adjust as needed.
Relaxation before bed: Try guided meditation, doodling, colouring, or listening to calming music to quiet the mind and prevent overthinking. Focus on single-tasking.
For Both
Cold Exposure: End your shower with 30–60 seconds of cold water to improve insulin sensitivity and reduce inflammation, slowly and with a smile on your face!! This increases your resilience and encourages mitochondrial health. Associated thoughts count!
Stress Management: Chronic stress raises cortisol, which worsens insulin resistance and the progesterone: oestrogen ratio. Try diaphragmatic breathing, yoga, or meditation daily.
Natural light: Spend 20–30 minutes outdoors daily, preferably in nature, to regulate circadian rhythms and reduce stress.
Digital Sunset: Avoid screens 1–2 hours before bed to support melatonin production.
3. Supplements: Targeted Support for Hormones and Metabolism
For Insulin Resistance
Berberine: (with meals). Studies show it is effective for lowering blood sugar (5).
Alpha-Lipoic Acid (ALA): improves insulin sensitivity and reduces oxidative stress (6).
Chromium: enhances insulin action (7), especially if your diet is poor in chromium-rich foods (wholegrains, nuts, meat).
Inositol: (myo-inositol : D-chiro-inositol) supports insulin signalling and may reduce sugar cravings (8).
For Perimenopause
Magnesium Glycinate or Bisglycinate: before bed to calm the nervous system and improve sleep.
Vitex (Chasteberry): can help balance progesterone and oestrogen (best taken in the morning) (9).
Black Cohosh: may reduce hot flashes and night sweats (avoid if you have liver issues).
Sage Leaf: as a concentrated tea to reduce sweating at least 1 -2h before bed (10).
For Both
Adaptogens such as Ashwagandha or Rhodiola help the body adapt to stress and support adrenal function.
Vitamin D3 + K2: to reduce inflammation and support hormone production, if you are deficient or if your time spent outdoors is reduced.
Omega-3s (EPA/DHA): to lower inflammation and support brain health.
Nootropics : making dietary and lifestyle changes requires a lot of brain energy, you might want to consider a nootropic herb like Ginkgo, Bacopa or Gotu kola.
Note: Always consult a healthcare provider before starting new supplements, especially if you’re on medication (e.g., blood pressure or diabetes meds).
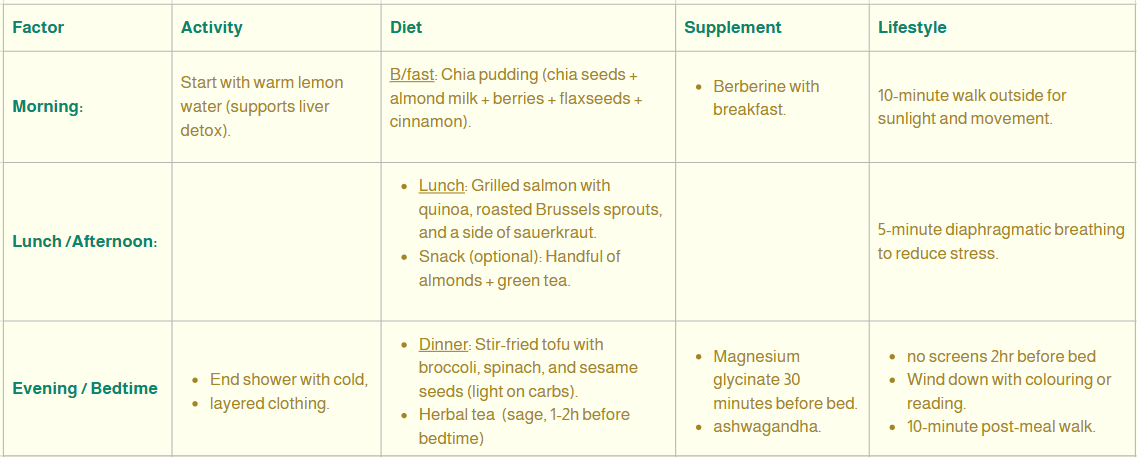
Putting it all together: A sample day
Here’s how you might structure your day to address both perimenopause and insulin resistance:
Sample day for information only. Supplements indicated here are for information only. Consult your naturopath for the supplements that will suit you best.
When to seek further support
While natural approaches can be highly effective, consider working with a naturopath or functional medicine practitioner if:
Your night sweats persist despite dietary and lifestyle changes.
You struggle to implement changes
You experience dizziness, heart palpitations, or extreme fatigue (could indicate blood sugar imbalances or thyroid issues).
You have a family history of diabetes or metabolic syndrome.
Final thoughts: Reclaim your nights
Night sweats don’t have to be an inevitable part of perimenopause—or a silent sign of insulin resistance. By addressing blood sugar balance, hormonal health, and stress, you can restore your body’s natural equilibrium.
Start with one or two changes (e.g., reducing evening carbs and adding magnesium) and track your symptoms. Small, consistent steps often yield the most sustainable results.
Remember: Your body is wise. Night sweats are the body’s way of signalling that something needs attention. Listen, nurture, and respond with kindness—because true wellness begins with self-care.
Have you tried any of these strategies? Which one resonates with you the most? Do not hesitate to contact me to share your experiences.
References
(1) Australian Institute of Health and Welfare. (2024). Diabetes: Australian facts. https://www.aihw.gov.au/reports/diabetes/diabetes/contents/summary
(2) Prior J. C. (2011). Progesterone for Symptomatic Perimenopause Treatment - Progesterone politics, physiology and potential for perimenopause. Facts, views & vision in ObGyn, 3(2), 109–120.
(3) Kaur, J., Gandhi, J., & Sharma, S. (2025). Physiology, cortisol. In StatPearls [Internet]. StatPearls Publishing.
(4) Garett, A. (2024). The Cortisol Connection to Perimenopausal Hormone Imbalance. https://drannagarrett.com/cortisol-connection-perimenopausal-hormone-imbalance/
(5) Xie, W., Su, F., Wang, G., Peng, Z., Xu, Y., Zhang, Y., Xu, N., Hou, K., Hu, Z., Chen, Y., & Chen, R. (2022). Glucose-lowering effect of berberine on type 2 diabetes: A systematic review and meta-analysis. Frontiers in Pharmacology, 13, 1015045. https://doi.org/10.3389/fphar.2022.1015045
(6) Pourmasoumi, M., Hadi, A., Mohammadi, H., Seyed Hadi, M., Moradi, A., & Khorrami, M. (2022). Efficacy and safety of oral alpha-lipoic acid supplementation for type 2 diabetes management: A systematic review and dose–response meta-analysis of randomized trials. Endocrine Connections, 11(10), 1234–1256. https://doi.org/10.1530/EC-22-0322
(7) Balk, E. M., Tatsioni, A., Lichtenstein, A. H., Lau, J., & Pittas, A. G. (2007). Effect of chromium supplementation on glucose metabolism and lipids: A systematic review of randomized controlled trials. Diabetes Care, 30(8), 2154–2163. https://doi.org/10.2337/dc06-0996
(8) Zarezadeh, M., Hamedi, A., & Ghaffari, M. P. (2022). Inositol supplementation and body mass index: A systematic review and meta-analysis of randomized clinical trials. Obesity Science & Practice, 8(3), 275–285. https://doi.org/10.1002/osp4.569
(9), (10) Fisher, C. (2018). Materia medica of Western herbs. Aeon; Hechtman, L. (2019). Clinical naturopathic medicine: Vol. Rev. ed (2nd ed.). Elsevier.